M Luperto, M Bouard, S Mongodi, F Mojoli, B Bouhemad Critical Care 2018, 22(Suppl 1):P211 Introduction: Diaphragm ultrasound (DUS) easily identifies diaphragmatic dysfunction (DD) in ICU patients [1], a potential cause of weaning failure (WF). Methods: Prospective observational monocenter study. We enrolled adults ICU patients at day 1 after surgery, extubated, with no neuromuscolar diseases. […]
S. Mongodi, F. Mojoli, G. Via, G. Tavazzi, F. Fava, M. Pozzi, G. A. Iotti, B. Bouhemad
Introduction: Weaning failure (WF) from mechanical ventilation (MV) may be due to lung derecruitment, cardiac dysfunction and respiratory muscles weakness. Transthoracic echocardiography (TTE) [1], lung ultrasound (LUS) [2] and diaphragm ultrasound (DUS) [3] have shown their value in early identification of the failing patients separately. A combination of TTE, LUS and DUS could improve the identification of failing patients and of WF etiology [4]. We aimed to estimate the value of a combined ultrasound assessment (heart-lung-diaphragm) to early identify patients at high risk of WF from MV.
Methods: Prospective observational multicenter international study including all patients undergoing a 30’ spontaneous breathing trial (SBT) before extubation. Patients with neuromuscular diseases and MV <48 hours were excluded. TTE and LUS were performed before SBT and at its end; DUS at beginning and end of SBT. TTE included: MAPSE (mitral annulus plane systolic excursion), EF% (ejection fraction), E/A, E/Ea. We computed LUS score (0–36) [2]. DUS assessed diaphragm excursion. Extubation was considered as failed in case of reintubation, non-invasive ventilation or death within 48 hours. We used classical criteria for SBT failure. Extubation was decided by an independent operator.
Results: We enrolled 18 patients (age 77.7 ± 11.4 yrs, BMI 29.9 ± 7, SAPSII 54.4 ± 17.4, MV length 9.5 ± 7.3 days). 6 patients (33%) failed the SBT and were not extubated. 12 patients (67%) were extubated; 5 failed. Two populations were identified: WF (failed SBT or extubation) and weaning success (WS). LUS: SBT-LUS was higher than MVLUS in the whole population (17 ± 4 vs. 12 ± 3; p = 0.019); this was more remarkable in WF (20 ± 3 vs. 11 ± 3; p = 0.0004). SBT-LUS was higher in WF vs. WS (20 ± 3 vs. 13 ± 4; p = 0.03). SBT-LUS predicted SBT and weaning failure (respectively AUC 0,877 and AUC 0,883). TTE: E/A and E/Ea (both MW and SBT) did not predict WF, extubation failure nor SBT-failure. MV-MAPSE predicted WF (AUC 0,833); if < =10 mm it predicted WF with sensitivity 0.67 and specificity 1. SBTMAPSE predicted extubation failure (AUC 0.833). DUS: No correlation between diaphragm excursion and WF was identified.
Conclusions: LUS and MAPSE seem to be the most useful parameters to predict weaning failure.
References 1. Caille et al., Crit Care 2010 2. Soummer et al., Crit Care Med 2012 3. Kim et al., CCM 2011 4. Mongodi et al., Crit Care Med 2013
Grant The research project received the ESICM Clinical Research Award 2015.
Pag. 30 From Critical Care
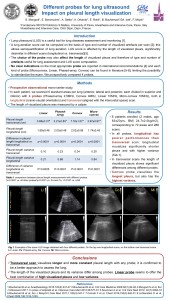
Different probes for lung ultrasound – impact on pleural length visualization
S. Mongodi , E. Bonvecchio , A. Stella , E. Roldi , A. Orlando, M. Luperto, B. Bouhemad, G. A. Iotti, F. Mojoli
Critical Care 2017, 21(Suppl 1):P84, 32
Introduction: Lung ultrasound (LUS) is a useful tool for lung diseases’ assessment and monitoring [1]. A lung aeration score can be computed on the basis of type and number of visualized artefacts per scan [2]; this allows semiquantification of lung aeration. LUS score is affected by the length of visualized pleura, significantly different in different scans (longitudinal (Long) vs. transversal (Transv)) [3]. The choice of the probe may also affect the length of visualized pleura, and therefore type and number of artefacts useful for lung assessment and LUS score computation. No clear indications on the most appropriate probe are reported in recommendations [4] and different kinds of probe (microconvex-Mi, linear-Li, phased-array-Pa, convex-Co) can be found in literature [5–8], limiting the possibility to standardize the exam. We prospectively compared 4 probes.
Methods: Prospective observational monocenter study. In each patient, we scanned 6 standard areas per lung (anterior, lateral, posterior, each divided in superior and inferior) with 4 probes (Pa 2.5 MHz, Co 4 MHz, Li 10 MHz, Mi 10 MHz), in Long (craniocaudal orientation) and Transv (aligned with intercostal space) scan. The length of visualized pleura was measured by a caliper.
Results: We enrolled 6 patients (2 males, age 63 ± 23 yrs, BMI 24.7 ± 2.0 kg/m2), corresponding to 72 areas and 288 scans. In all probes, Long has poorer performances than Transv scan: it visualizes significantly shorter pleura with higher pleural length variance (Table 12). In Transv, the length of visualized pleura shows significant differences among different probes. Co visualizes the longest pleura, but also has the highest pleural length variance.
Conclusions: Transv visualizes longer and more constant pleura with any probe; it’s confirmed to be a better approach to assess the lung. The length of visualized pleura and its variance differ among probes; linear probe seems to offer the best combination of high visualized pleura and low pleural length variance.
References 1. Bouhemad B et al., Anesthesiology 2015,122(2):437–47 2. Bouhemad B et al., Crit Care Medicine 2008;38(1),84–92 3. Mongodi S et al., Eur J Ultrasound 2016; In press 4. Volpicelli et al., Intensive Care Med 2012;38:577–91 5. Soummer A et al., Crit Care Med 2012, 40(7):2064–72 6. Bouhemad B et al., Am J Resp Crit Care Med 2011;1;183(3):341–7 7. Corradi F et al., Chest 2016;150(3):640–51 8. Lichtenstein D et al., Chest 2009;136:1014–1020
From Critical Care, Pag. 32 P84
Bianzina S, Cornara P, Rodi G, Tavazzi G, Iotti GA, Mojoli F, Braschi A Intensive Care Medicine Experimental 2016, 4(Suppl 1):27;116 Introduction: Pulmonary alveolar proteinosis (PAP) is a rare disorder characterized by a perturbation in surfactant homeostasis, resulting in its accumulation within alveolar spaces, with a consequent development of severe hypoxemia. Whole lung lavage (WLL) is a complex […]
Mojoli F, Orlando A, Bianchi I, Torriglia F, Bianzina S, Pozzi M, Iotti GA, Braschi A, PLUG Working Group Intensive Care Medicine Experimental 2016, 4(Suppl 1):27;597 Introduction: Patient-ventilator asynchronies are associated with poor outcome. It was suggested that bedside analysis of ventilator waveforms may help detecting different types of asynchrony and setting properly […]
Mojoli F, Orlando A, Bianchi I, Torriglia F, Bianzina S, Pozzi M, Iotti GA, Braschi A, PLUS Working Group Intensive Care Medicine Experimental 2016, 4(Suppl 1):27;595 Introduction: Standard waveforms displayed on the ventilator screen may help detecting whether the ventilator is switching form inspiration to expiration at the right time, thus allowing appropriate […]
Mojoli F, Torriglia F, Giannantonio M, Orlando A, Bianzina S, Tavazzi G, Mongodi S, Pozzi M, Iotti GA, Braschi A, PLUG Working Group Intensive Care Medicine Experimental 2016, 4(Suppl 1):27; 534 Introduction: A calibration procedure has been recently proposed to obtain reliable esophageal pressure (Pes) measurements in mechanically ventilated patients [1]. This procedure […]
F Mojoli, M Pozzi, S Bianzina, G Tavazzi, A Orlando, S Mongodi, F Torriglia, A Braschi Intensive Care Medicine Experimental 2015, 3(Suppl 1):A998 doi:10.1186/2197-425X-3-S1-A998 From ESICM LIVES 2015 Berlin, Germany. 3-7 October 2015 Full text attached: 2015, F. Mojoli, Automatic monitoring of plateau and driving pressure during pressure and volume controlled ventilation, ICMX http://www.icm-experimental.com/content/3/S1/A998 Share this:
F Mojoli, S Bianzina, I Bianchi, G Tavazzi, S Mongodi, M Pozzi, A Orlando, A Braschi Intensive Care Medicine Experimental 2015, 3 (Suppl 1):A514 doi:10.1186/2197-425X-3-S1-A514 From ESICM LIVES 2015 Berlin, Germany. 3-7 October 2015 Full Text Attached: 2015, F. Mojoli, Artificial lung gas exchanges depend on ECMO settings, ICMX http://www.icm-experimental.com/content/3/S1/A514 Share this:
F Mojoli, S Bianzina, L Caneva, G Tavazzi, S Mongodi, M Pozzi, A Orlando and A Braschi Intensive Care Medicine Experimental 2015, 3(Suppl 1):A506 doi:10.1186/2197-425X-3-S1-A506 Full text attached: 2015, F. Mojoli, Temperature monitoring during ECMO- an in vitro study, ICMX http://www.icm-experimental.com/content/3/S1/A506 Share this: